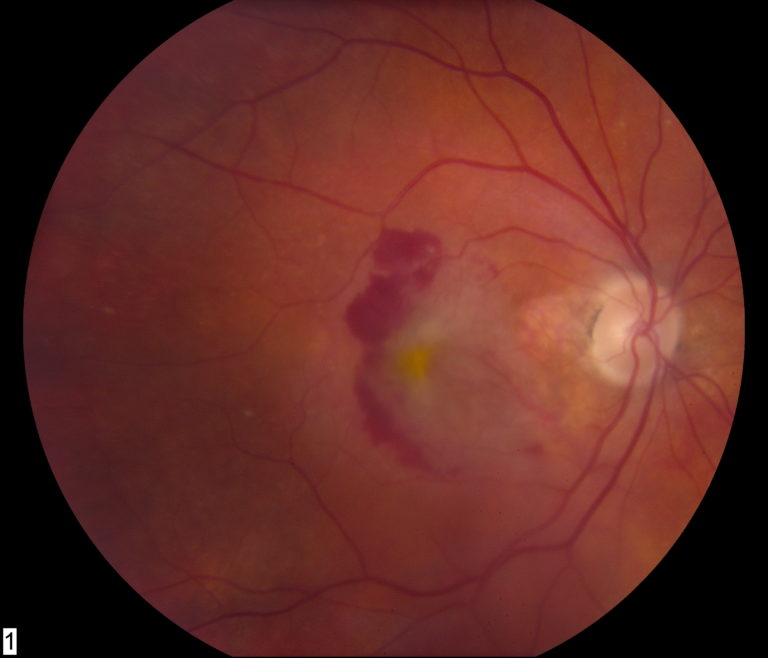
Macular Degeneration (AMD)
Macular degeneration (also known as AMD – age related macular degeneration) is a disease of the retina that is characterized by a breakdown of the central part of the retina or macula. The macula is the only part of the retina that is responsible for acuity (sharp vision) and color vision. Accordingly, it is the part of the eye the uses the most energy to work. Over time, we begin to see deposits in the tissue under the retina indicating that the body is no longer able to clear the debris of normal activity.
Risk Factors for Macular Degeneration
These deposits are called Drusen. Drusen usually become noticeable to the doctor on examination after the age of 65. This is the so called dry form of macular degeneration and is the most common form of the disorder. Risk factors for macular degeneration include:
Age greater than 65
Caucasian race
Female gender
Blue eyes
Smoking
A history of hypertension
Sun exposure
and RARELY family history

Two Types of AMD
85% of patients with macula degeneration will have the dry type. Dry AMD may be asymptomatic for years. Symptoms usually occur when the macula begins to thin or atrophy. These symptoms are usually a gradual reduction in the central vision. Currently there are no available treatments to restore the thinned retina. Patients are advised to quit smoking, use antioxidants (AREDS) and wear sunglasses, to slow down the breakdown process. Regular checkups and testing the central vision with an Amsler grid is important.
The wet form of AMD is characterized by the growth of abnormal blood vessels under the retina. These blood vessels grow through the areas that were weakened by the deposits (Drusen) in the retina and may lead to bleeding and the formation of scar tissue under the retina. The patient will usually notice a sudden and abrupt change in vision with distortion as the prominent symptom. This is the most aggressive form of the disease, which if left untreated, may lead to permanent scarring and subsequent central blindness. This form (wet AMD) requires prompt evaluation and treatment by a retinal specialist.
Treatment for Macular Degeneration
Treatment for AMD has made significant improvement recently. Previous treatment, including laser, photodynamic therapy, and radiation were all less than optimal and almost all patients STILL LOST VISION! Today, with new medications like Eylea and Avastin, we are able to stabilize the vision in 95% of patients and IMPROVE THE VISION in up to 40% of patients. Patients are treated with an injection of the drugs to arrest the growth of the abnormal blood vessels. It is important to know that this treatment is NOT A CURE and patients will require repeat treatment in most cases indefinitely. Current research continues to evolve better drugs and drug delivery devices to improve the available treatment options.
Keith Warren, M.D.
Retina Specialist
Board Certified Ophthalmologist
Overland Park and Kansas City